Overview of Osteoporosis:
Osteoporosis means porous bones. The word Osteo refers to “the bones” and porosis means “pores”. So, osteoporosis occurs when there’s a higher breakdown of bone in comparison to the formation of new bone. And it also results in porous bones which mean is a decrease in bone density to the point of potential fracture.
Structure of bone:
A bone cross-section contains a hard external layer known as the cortical bone. It also contains a softer internal layer of spongy bone or trabecular. The trabeculae act as a framework of beams the main function Is to give structural support to the spongy bone. The cortical bone is compose of osteons are pipe-like functional units, which run through the length of the bone. The Osteons center contains hollow spaces called Haversian canals. They contain the blood supply and innervations for the bone cells. Concentric lamellae are present around the Haversian canals that look a bit like tree rings.
The lamellae have two parts organic and organic. The organic part is mostly called collagen and the other part that is inorganic is called hydroxyapatite. The inorganic part is mostly calcium phosphate. There are spaces between neighboring lamellae that are call lacunae. They mostly contain bone cells that are called osteocytes. Firstly, bone appears unchanging and inert. But it is a very dynamic tissue. In the remodeling process, spongy bone is replaced every 3 to 4 years and compact bone is replaced every 10 years.
Bone remodeling:
Bone remodeling has two steps. Bone resorption, when specialized cells name as osteoclasts break down bone, and bone formation, which is when another type of cells called osteoblasts form new bone.
What influences bone remodeling?
Bone remodeling is highly dependent on serum calcium levels. The calcium level is maintain by a balance between calcitonin, parathyroid hormone, or PTH and vitamin D. Parathyroid hormone in the body is produce by the parathyroid glands of the body. It is mostly made in response to low serum calcium in the bones. So, its main function is to increase bone resorption to release calcium into the bloodstream.
On the other hand, thyroid gland is produced calcitonin in response to high serum calcium. So, it is against the action of PTH. Therefore it promotes bone formation and also decreases bone resorption. In the end, vitamin D promotes calcium absorption in the gut. So it increases serum calcium and promotes bone formation.
The balance of these regulatory factors makes a peak bone mass. It is usually by age of 20 to 29. And this process usually occurs earlier in females than in males.
Factors that determine the peak bone mass:
- Genetics (for example, people of African descent tend to have greater bone mass)
- Nutrition (meaning adequate vitamin D intake increases bone peak mass).
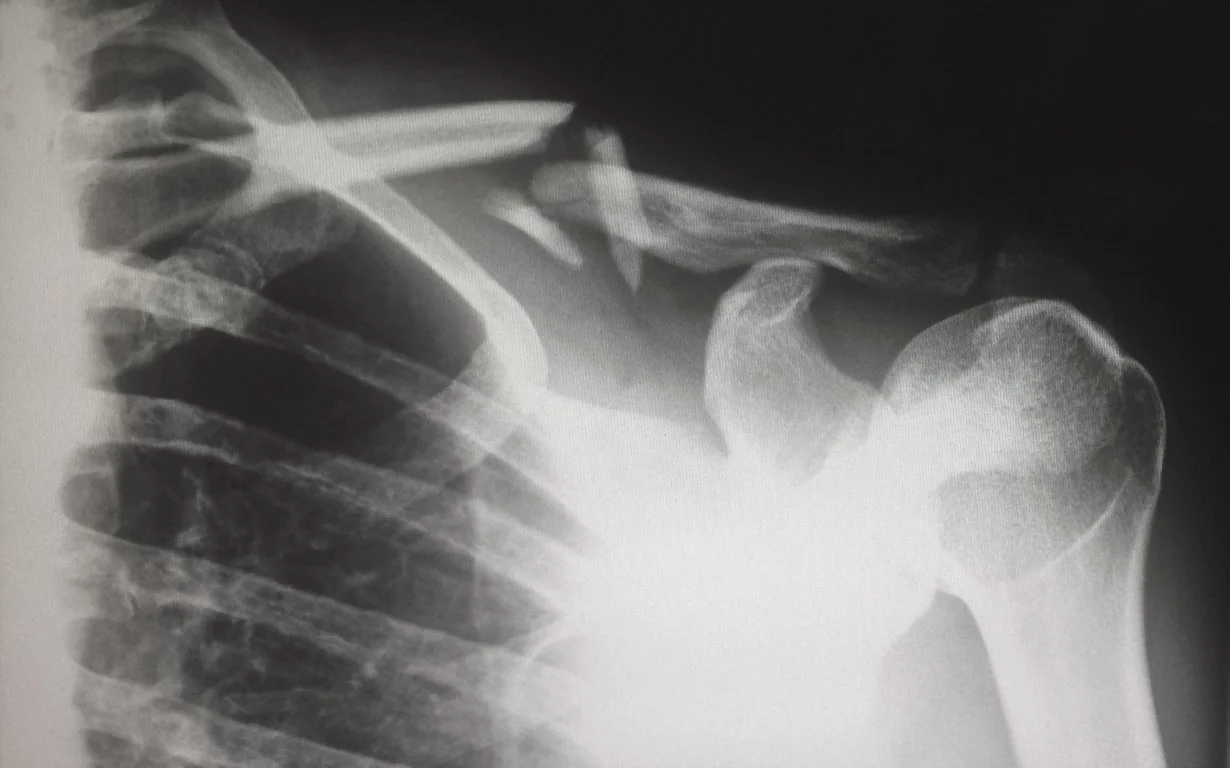
Finally, strength training increases peak bone mass. The hormones like estrogens and androgens are inhibiting bone resorption. when osteoclasts break down bone faster than the osteoblasts can rebuild, it results in the lowering of the bone mass and eventually in osteoporosis So, with osteoporosis, abnormal findings include fewer trabeculae in the spongy bone and thinning of the cortical bone, as well as the widening of the Haversian canals. The change in bone increases the risk of fracture. This is known as pathologic fractures or fragility. Some bones of body for example the shoulder blades, vertebrae and ribs consist of spongy bone. These spongy bones are at great risk of fragility fractures.
Factors that increase the risk of Osteoporosis:
Factors that increase the risk of osteoporosis and accelerate bone mass loss are:
- Low estrogen levels mostly occur after menopause and due to low serum calcium.
- Alcohol consumption
- smoking
- Drugs usage like glucocorticoids, which decrease calcium absorption from the gut through antagonism of vitamin D, and drugs like heparin and L-thyroxine.
- Physical inactivity is mostly observe in astronauts in zero-gravity. These astronauts don't use their musculoskeletal system hardly in sky as compared to earth. As a result, due to lack of stress bone deposition and resorption increase.
Name the diseases that increase the risk of osteoporosis?:
There are many diseases that can associate with osteoporosis like:
- Turner syndrome
- Hyperprolactinemia
- Klinefelter syndrome
- Cushing syndrome
- Diabetes mellitus
Type of Osteoporosis:
The two most common types of osteoporosis are name as:
- Postmenopausal Osteoporosis
- Senile Osteoporosis
1. Postmenopausal osteoporosis:
In this type estrogen levels decreases and lead to increased bone resorption.
2. Senile osteoporosis:
In this case osteoblasts gradually lose the ability to form bone. And the osteoclasts keep doing their thing nonstop.
What are Symptoms of Osteoporosis?
People with osteoporosis usually do not have visible symptoms. It mostly diagnoses when a fracture occurs. The most common type of fractures is a compression fracture, also known as a vertebral fracture. So, it occurs when one or more bones in the spine weaken and shatter. The vertebral fracture causes height loss, back pain, and a hunched posture.
Distal radius fractures and femoral neck fractures also occurs and they are also associate with postmenopausal osteoporosis.
Diagnosis of Osteoprosis? :
Osteoporosis is usually diagnose by bone density tests in which dual-energy X-ray absorptiometry or DEXA scan involve. In this test comparison of an individual's bone density to that of a normal adult occurs. If A T score is less than or equal to -2.5, it is diagnostic of osteoporosis.
Treatment for osteoporosis:
It usually relies on Bisphosphonate drugs that involve risedronate and Alendronate. If osteoporosis is severe, Teriparatide drug which is a recombinant parathyroid hormone can be used. Because parathyroid hormone stimulates bone resorption. It is observe that intermittent injections with Teriparatide can activate osteoblasts more than osteoclasts and as a result bone formation increases.
And a drug name Thiazide diuretic like Hydrochlorothiazide can also treat osteoporosis. The main function of Hydrochlorothiazide is to boost calcium retention in the kidney and it directly stimulates osteoblast differentiation. As a result, mineral bone loss decreases. Finally, medications like Denosumab which is a monoclonal antibody can also inhibit osteoclasts. Another drug name Raloxifene is a selective estrogen receptor modulator use for postmenopausal osteoporosis.